Massage for Athletes
Massage Therapists Benefit Athletes Performance
Athletes have much in common with massage therapists – some massage therapists even consider ourselves athletes. We regularly perform complex movements over an extended period of time, for both work and enjoyment. Massage therapists and athletes alike have an understanding of anatomy via training, performing, and education. Both groups often feel exhaustion from overuse, and have developed a variety of methods to improve recovery. With these similarities in mind, massage therapists have a strong foundation with which to develop healing techniques. The work of massage therapists benefit athletes performance – on and off the field.
Impact of Massage on Athlete Physicality
The most obvious area where massage therapists help athletes, is in their physicality and specialized movements. Whether a professionally trained Olympian, or a desk-piloted weekend warrior, performing in a sport or event will push one’s body to its limits.
Massage therapists consider many aspects of someone’s lifestyle to uncover the best method of treatment. A high-level athlete with a dedicated training regimen may benefit from myofascial release and muscle rolling techniques, whereas an aircraft technician, whose weekend pick-up games conclude with beer and pizza, may have different needs altogether.
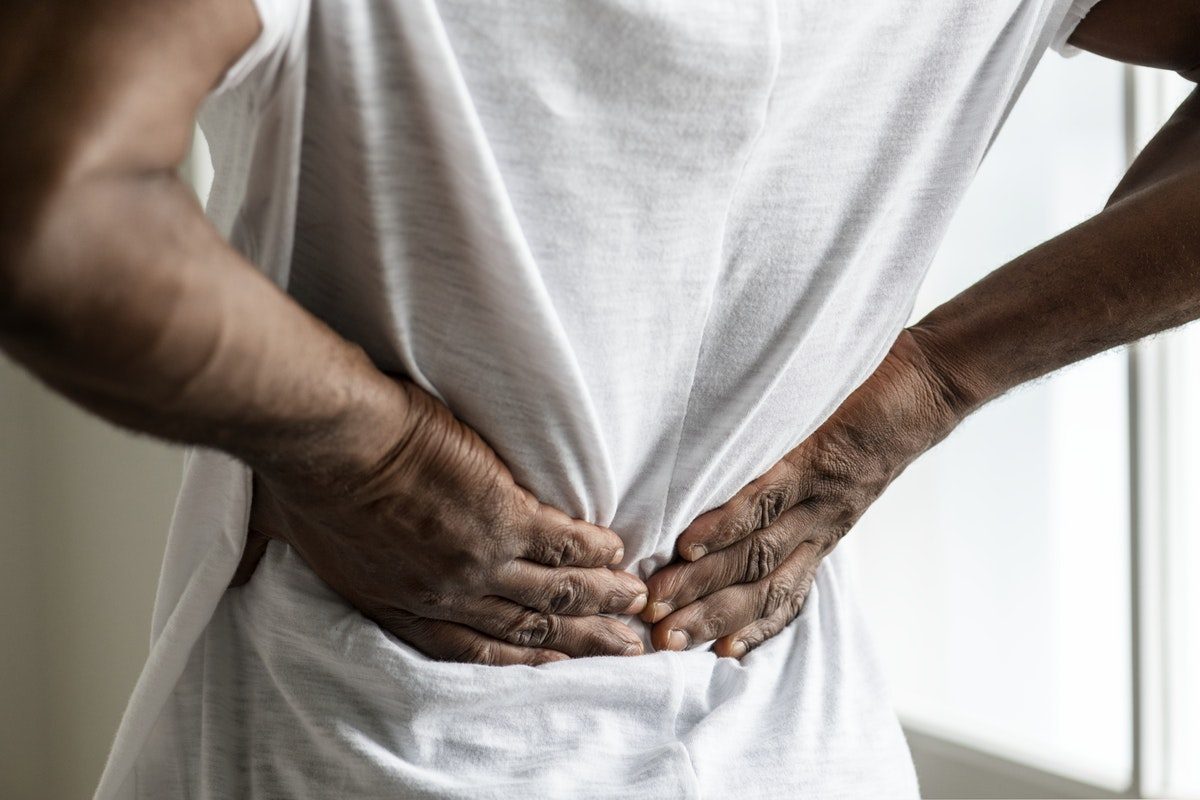
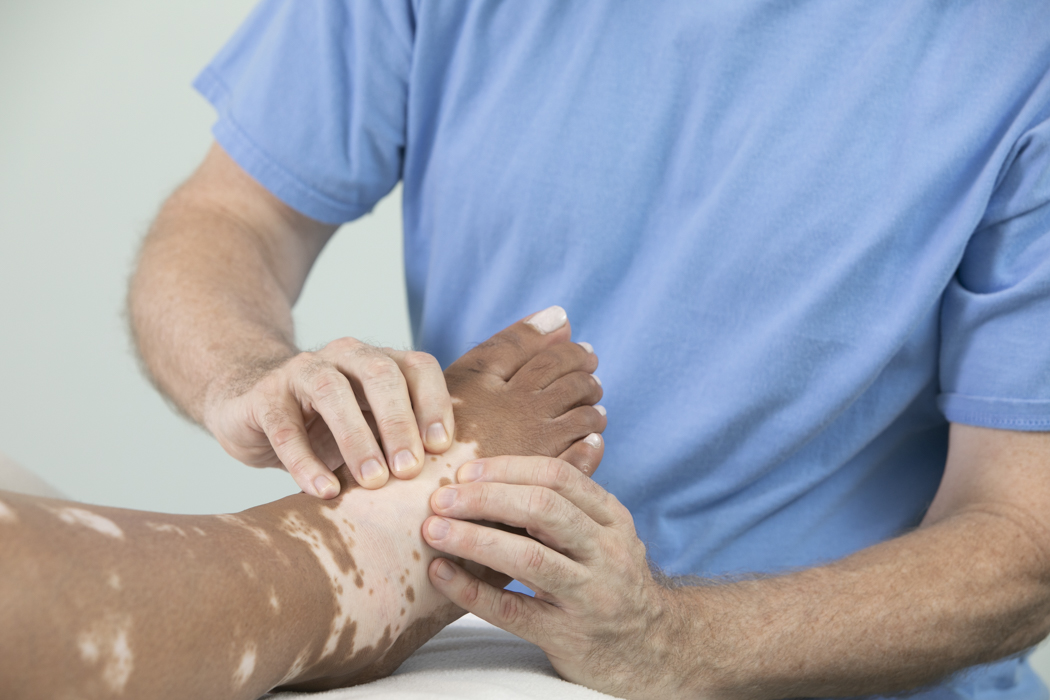
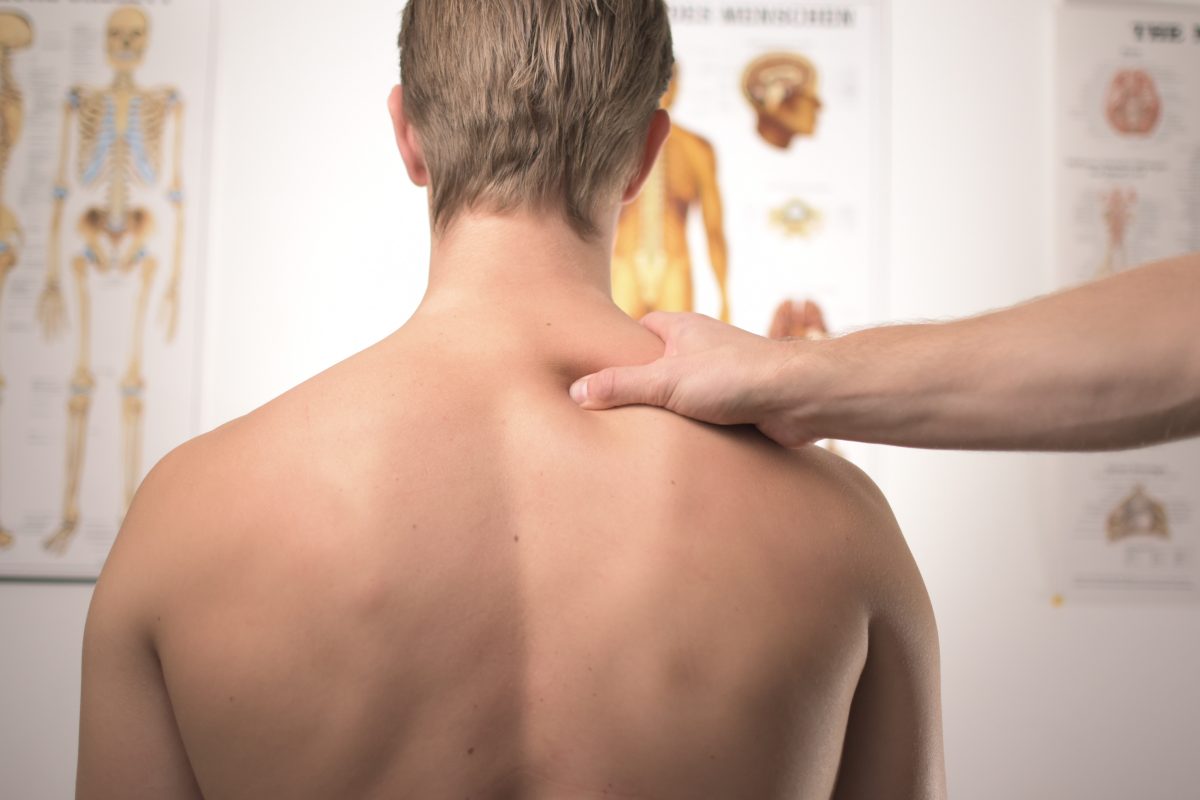
Massage therapists can apply sports massage before, during, and after an event, in order to help decrease pain and improve mobility for an athlete. This often includes releasing a tight muscle, which has become dysfunctional due to extended overuse. Massage therapists also help develop recovery plans around an athlete’s schedule, to help maintain their health away from the table. By assisting an athlete’s body to move more comfortably and functionally, massage therapists can be pivotal to an athlete’s success.
Impact of Massage on Athlete Mentality
Another way massage therapists help athletes, and one which is often overlooked, is in the athlete’s mentality. Athletes undergo emotional stress that can often interfere with their performance, training, and/or recovery. Sometimes this stress may be linked to a shortcoming in their training, or it can be totally unrelated (Mr. Whiskers’ birthday is coming up, and his tuna surprise must be perfect).
Massage therapists are typically aware of the focus and clarity required to achieve high-level goals, athletic or otherwise. As such, they are trained to facilitate an athlete’s relaxation during a session. Time spent on the (massage) table can benefit athletes, allowing them to check in mentally, and take note of the ways in which their health relates to the ability to reach their performance goals. Massage therapists will listen to their clients’ goals and needs, and are able to adjust their work accordingly. Sometimes a sports massage will diverge halfway through the session; what starts as a general tune-up transitions into a targeted focus session. Client-centered bodywork can be a missing ingredient for many athletes working to develop their mind-body connection.
Conclusion
Massage therapists can benefit their athlete clients in many ways. Whether they are looking to reduce joint pain, hit their PRs, or need extra mobility in their shoulder to perfect their lay-up, massage therapists can help. If a distressed athlete wants to rework their training schedule, or a new parent, short on sleep, wants to mentally prepare for a half-marathon this weekend, massage can help. Massage therapists are lucky to work with many people from all walks of life, and among those to which it may be the most beneficial, athletes.